Anal Sac Adenocarcinoma
By Dr. Suzanne Rau, DVM, DACVIM (Oncology) | Oncology
Apocrine gland anal sac adenocarcinomas (AGASACA) comprise about 17% percent of perianal malignancies, and 2% of all skin and subcutaneous tumors. The average age at diagnosis is nine to eleven years.
DIAGNOSIS AND STAGING
Some dogs with AGASACA present with signs related to the mass itself, such as a swelling in the perianal region, a mass palpated on routine rectal exam, scooting, or straining to defecate. Other dogs may present for signs indirectly related to the mass if the tumor is causing hypercalcemia, which is reported to occur in about 25% of dogs with AGASACA. These hypercalcemic dogs may be polyuric and polydypsic.
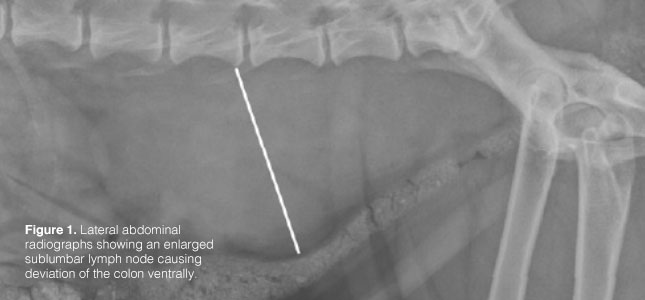
The reported rate of metastasis at the time of diagnosis ranges from 50-80%. Therefore, prior to surgery and other therapies, staging with three view chest x-rays and an abdominal ultrasound are recommended. The sublumbar lymph nodes are one of the most common sites for metastasis (Figure 1). This lymph center includes the medial iliac, hypogastric, and sacral lymph nodes and is located within the caudal abdomen and pelvis. More common distant metastatic sites include the spleen, liver, and lungs. Rarely, regional bone metastasis or direct extension of tumor from the sublumbar lymph nodes to the lumbar vertebrae can occur.
TREATMENT
Treatment for this disease involves both local control of the primary mass itself, as well as controlling tumor metastasis.
SURGERY
Surgery to remove the primary mass in the anal region and/or removal of enlarged sublumbar lymph nodes within the abdomen is often the first step. Ideally these tumors should be removed with wide margins, however, given their close proximity to the rectum and important neurovascular structures, resection is often marginal.
Risk of incontinence is low and typically transient with unilateral anal sacculectomy, and only slightly increased for bilateral anal sacculectomy; bilateral anal sac tumors have been reported in approximately 10% of cases. Masses that are still contained within the anal gland are generally easier to remove than those that have ruptured out of the capsule and started invading the muscle of the anal sphincter.
Removal of metastatic lymph nodes has been shown to increase survival time in many cases. Removal can be challenging due to their caudal location within the abdomen at the aortic bifurcation. However, they are usually well encapsulated and can be successfully removed without major complications.
RADIATION THERAPY
Definitive Radiation
In cases where some cancer cells may have been left behind after surgery, regrowth of the primary tumor could occur in the future. Definitive radiation therapy may be recommended post-operatively in patients. This is radiation treatment given in an attempt to eliminate any residual disease both at the peri-anal site and the draining abdominal lymph node bed. The intent of definitive radiation is long-term tumor control, and typically consists of daily treatments (Monday through Friday) of a small dose of radiation for 3-4 weeks. Dogs are anesthetized for a short period of time during the treatments.
Side effects include a radiation burn to the sensitive skin at the peri-anal site, as well as diarrhea due to radiation of the sublumbar lymph node bed, which lies adjacent to the colon. Although the side effects can be severe, they typically heal within one month after finishing therapy. Some dogs, however, may experience long term diarrhea or straining when defecating.
PALLIATIVE RADIATION
An option for tumors that are not amenable to surgical removal, or start to recur in the future is a different form of radiation therapy called palliative radiation. This type of radiation similarly targets the local mass and draining lymph nodes. However, due to the difference in dose administration, it is much less likely to cause acute adverse side effects in patients. This type of treatment may be given once a week for 4-6 treatments, or daily Monday through Friday for one week. In a small retrospective study, about 50% of dogs experienced shrinkage of their anal sac masses or lymph nodes, while nearly 90% had at least stabilization of their disease. The duration of these responses was about six months.
CHEMOTHERAPY
Chemotherapy may also be recommended post-operatively, as these tumors often metastasize to other areas of the body, including the local lymph node and lungs. More common chemotherapy drugs used to treat AGASACA include carboplatin and mitoxantrone. Protocols may vary, but often include 4-6 treatments given every three weeks.
Possible side effects of chemotherapy include vomiting, diarrhea, or inappetence that can occur in a 3-5 day window after chemotherapy administration. Suppression of the bone marrow can also occur between one and three weeks after treatment depending on the drug given. Rarely, dogs have side effects that are severe enough to warrant hospitalization; this happens in about 5-10% of patients. Chest x-rays and abdominal ultrasounds are usually repeated for monitoring during therapy.
PALLADIA
A newer option for the treatment is an oral medication called Palladia. This is a drug that was originally approved for treatment of mast cell tumors, though has exhibited responses in other tumor types as well, including AGASACA. It is reported to have anti-tumor activity as well as act as an antiangiogenic drug. Side effects of Palladia are primarily gastro-intestinal, though immune suppression can also be seen. While a pet is on Palladia, we recommend periodic monitoring of bloodwork to evaluate for any adverse effects. This drug is given continuously on an every other day or Monday, Wednesday, Friday basis until it is no longer effective. This treatment is often reserved for tumors that cannot be removed, recur, or have started to spread elsewhere since it needs to be given continuously for as long as it remains effective.
There are several retrospective studies evaluating the use of Palladia for the treatment of AGASACA. In one report, 25% of dogs experienced shrinkage of their disease, while 88% had at least stabilization of their cancers. In a second report, 62% of dogs experienced shrinkage of their disease, while 75% has at least tumor stabilization. In this study, the median progression free interval was 328 days.
SUPPORTIVE THERAPIES
Medications such as stools softeners and anti-inflammatories can also be added for patients who have difficulty defecating due to the presence of the primary mass or enlarged lymph nodes in the region. This can offer relief for many patients by allowing them to defecate more easily.
Symptoms of hypercalcemia can be controlled with fluid therapy and prednisone, or calcium lowering drugs like bisphosphonates.
PROGNOSIS
The overall median survival time for AGASACA is about 18 months with various forms of treatment. However, many factors including characteristics of the tumor, results of staging tests, and therapy options chosen by the owner can all impact prognosis.
Factors including a larger tumor size at the time of removal (>10cm2), the presence of metastasis, and hypercalcemia on blood work have been associated with a more guarded prognosis. Dogs with tumors >10cm2 had median survival times of about 9 months compared to about 19 months for dogs with smaller tumors. Patients with an elevated calcium levels had median survival times of 8.5 months compared to about 19 months for patients with normal calcium levels.
Surgical intervention has repeatedly been shown to play an important factor in prognosis. Dogs treated with surgery to remove their tumors have a more favorable outcome than dogs with tumors that were not, or could not be removed. Even when lymph nodes are affected, surgery to remove these lymph nodes along with the primary tumor can result in a median survival time of over two years. If a tumor is found to recur locally or metastasize to lymph nodes in the future, a second surgery can result in a median of 283 days of additional survival time. Dogs treated most aggressively with a combination of surgery, radiation therapy, and chemotherapy had a median survival time of over two years in one report.
CONCLUSIONS
Although AGASACAs raise the concern for both the control of the local tumor, as well as the control of distant cancer metastasis, there are many therapy options available.
The prognosis can be favorable with multimodality treatments. However, even when an owner elects against more aggressive treatment modalities such as surgery and radiation therapy, medical therapies can often help to control a tumor and keep a dog comfortable for a period of time.
